- Birth control
- IUD
IUD
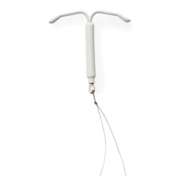
What is the IUD?
The intrauterine device (IUD) is a small, T-shaped piece of plastic that you can have a health care provider put inside your uterus. The IUD makes it harder for sperm to move efficiently, preventing it from fertilizing an egg. In the U.S., there are five brands of IUDs available: Kyleena, LILETTA, Mirena, Paragard, and Skyla.
IUDs can offer years of protection from pregnancy. How long they last depends on the type you get. Some last for up to three years and others last for up to 12 years. If you want to get pregnant or simply want to switch to a different method of birth control at any time, you can have the IUD removed. And if you have plans to get pregnant in the future, don’t worry—having an IUD now doesn’t affect your fertility in the future.
While the IUD is safe and super effective at preventing pregnancy, it doesn’t offer protection against sexually transmitted infections (STIs). For STI protection, you can use condoms, internal condoms, dental dams, gloves, and/or PrEP (pre-exposure prophylaxis, which lowers the risk of getting HIV from sex).
Three types of IUDs (LILETTA, Mirena, and Paragard) can also be used as emergency contraception if you get them within five days of having unprotected sex. These three types of IUDs are the most effective methods of emergency contraception, preventing pregnancy in over 99% of cases.
Quick Facts
-
Effectiveness
The IUD is super effective—one of the most effective birth control methods.
Perfect use: Over 99 % effective
Typical use: Over 99% effective
What are perfect use and typical use?
-
Hormones
There are hormonal and non-hormonal versions.
-
Side effects
With the hormonal IUD, you may have spotting between periods. With the non-hormonal IUD, you may have heavier periods.
-
Cost
Could range from $0 (with insurance) to $1300. There may be an extra cost for insertion and removal.
-
STI protection
The IUD doesn’t protect against STIs.
-
Ongoing effort
Once it’s in, there’s nothing for you to do. You can keep it in for years with no ongoing effort.
Types of IUDs

Hormonal IUD
There are four hormonal IUDs available in the U.S.—Kyleena, LILETTA, Mirena, and Skyla. All of them are made of plastic and release a small amount of the hormone progestin. Progestin is a synthetic version of progesterone, which is a hormone your body makes naturally. The main way progestin prevents pregnancy is by thickening cervical mucus to keep sperm from reaching the uterus.The hormonal IUD may change your periods, making them irregular, lighter, or shorter, or it may stop your period entirely.
How long you can use an IUD for depends on which one you get. The longest-lasting hormonal IUD (Mirena) prevents pregnancy for up to eight years, but you can have your IUD removed at any time.

Non-hormonal/copper IUD
There’s only one IUD without hormones available in the U.S. It’s called Paragard, and it’s made of plastic and a small amount of copper. Paragard works for up to 12 years, which is longer than any of the hormonal IUDs. It doesn’t change the timing of your periods or cause spotting (bleeding between periods), but it may cause increased bleeding and cramping when you get your period.

We can help you find an in person provider or online birth control delivery service.
find health care