Most methods will not cause weight gain. Most people gain weight over time (whether they are using birth control or not), so if you use birth control for a few years, weight gain may not be related to your birth control specifically. The exception to this is the shot. Some people who use the shot will gain some weight. However, the majority of people who use the shot don’t gain much.
- Birth control
- IUD
- FAQs
IUD
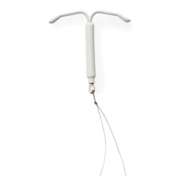
Will birth control make me gain weight?
Is it okay for me to take my own IUD out?
While some people choose to remove their own IUD, whether someone can successfully remove it depends on several factors, like the length of the IUD strings and the position of the cervix. If you try to remove your IUD and it won’t come out (or you can’t find the strings), contact a health care provider to help.
If you’re not happy with your IUD, going to your health care provider to get it removed will give you a chance to ask about other options for birth control. Or if you’re ready to get pregnant, you can talk with your provider about things you should do to prepare for a healthy pregnancy.
Want to learn more?
What is levonorgestrel?
Levonorgestrel is one of the longest-studied types of progestin which is the synthetic version of progesterone, a hormone made by the body. And all the scientific evidence to date shows it is super safe. It’s used in hormonal IUDs, some emergency contraception pills, and certain birth control pills.
How do I get birth control when I’m in the military?
If you are an active-duty member of the U.S. military, here’s some great news: you have access to a wide range of birth control methods covered under your TRICARE plan. The less great news: not all methods are offered at every military treatment facility (MTF), especially during deployment. That’s why even if you’re not sure you’ll need birth control, it’s a good idea to look into your options before you deploy—especially if you’re going overseas. We’ve laid out some tips and questions to think about so you can make an informed decision.
Want to learn more?
I heard the IUD is really expensive—how much does it cost?
If you don’t have health insurance, it’s true that the up-front cost of an IUD can be high, but because the IUD can last for years (3-12 depending on the type) even if you pay full price upfront it ends up being pretty cheap over time.
If that isn’t an option for you, the manufacturers of IUDs often offer discounts, and you can also check with the family planning clinics around you and find out if they offer discounts or payment plans for IUDs.
If you have health insurance—whether it’s through your parents, school, job, the Affordable Care Act (ACA) marketplace, or Medicaid—chances are good that you’ll be able to get an IUD with no out-of-pocket cost.
If you don’t have health insurance, it’s true that the up-front cost of an IUD can be high, but because the IUD can last for years (3-12 depending on the type) even if you pay full price upfront it ends up being pretty cheap over time.
If that isn’t an option for you, the manufacturers of IUDs often offer discounts, and you can also check with the family planning clinics around you and find out if they offer discounts or payment plans for IUDs.
Want to learn more?
Does the IUD protect against STIs?
No, the IUD does not protect against sexually transmitted infections (STIs). The best way to prevent STIs if you’re having sex is using a condom or the internal condom. Dental dams, gloves, some vaccines (HPV and hepatitis B vaccines) and daily medications, such as PrEP for the prevention of HIV, also offer STI protection. If you’re concerned about both pregnancy and STIs, you can these options for STI prevention at the same time as the IUD.
Want to learn more?
Is it safe to lose blood by spotting a lot?
Spotting refers to a small amount vaginal bleeding that is unpredictable or irregular and not related to your period. Spotting can be a normal side effect of some birth control methods, especially progestin-only ones like the shot, implant, mini-pill, and hormonal IUDs as well as with low-dose combination birth control pills. When birth control causes spotting, it isn’t dangerous and generally doesn’t make you lose that much blood, even though it might seem like it.
Will it hurt to have sex when I have an IUD inside me?
It shouldn’t. You may be a little bit sore immediately after insertion, but ultimately no. If your partner can feel the strings during sex, talk to a health care provider, they can trim the strings.
Want to learn more?
Can the IUD move out of place or fall out completely?
Sometimes. Occasionally it can work its way part or all of the way out, down through the cervix (the opening to the uterus)—that’s called expulsion. If that happens, it means you don’t have birth control any more, but it’s not usually dangerous. Expulsion is more common right after you have an IUD placed, if your IUD is placed right after giving birth or having an abortion after 14 weeks, if you have you haven’t been pregnant before, or are younger than 20 years old. If your IUD is expelled, you can have another IUD placed or start another method of birth control to prevent pregnancy.
In rare cases, the IUD can work its way up, and either get stuck in the muscle of the uterus or through the muscle of the uterus and into your abdomen—that’s called perforation. That really doesn’t happen often, less than 1 in 2,000 insertions. If it does happen, your IUD isn’t working as birth control and you may need surgery to remove it. While it’s not required, you can have a follow up visit with a provider to check the IUD 4-6 weeks after it’s placed or check the IUD strings in the vagina yourself: if you can feel the strings with your fingers, everything’s probably okay.
Want to learn more?
My IUD was expelled. Should I try again?
1. Haven’t been pregnant
2. Are younger than 20 years
3. Have a history of very heavy or very painful periods (though be mindful that these are reasons the hormonal IUD is recommended in the first place…)
4. Had the IUD put in right after giving birth or having an abortion after 14 weeks.
A partial expulsion may mean that the IUD was not quite in the right position: it may have been too low in the uterus and just worked its way out. This could be something that happened around the time of insertion, or may be related to the size, angle, or conditions like fibroids that can cause the uterus to have an irregular shape. For people who have an IUD expulsion, the chance of expelling a second IUD may be higher—in the 20% range (up to 30% in some studies).
If you want a second IUD after the first one came out, consider asking your health care provider about inserting the second IUD while using an ultrasound machine to make sure the IUD is inserted all the way to the top of the uterus where it belongs.
IUD expulsion (when part or all of the IUD comes out after it’s placed in the uterus) can occur in 2-10% of people in the first year after insertion. Expulsion can be more likely for people who:
1. Haven’t been pregnant
2. Are younger than 20 years
3. Have a history of very heavy or very painful periods (though be mindful that these are reasons the hormonal IUD is recommended in the first place…)
4. Had the IUD put in right after giving birth or having an abortion after 14 weeks.
A partial expulsion may mean that the IUD was not quite in the right position: it may have been too low in the uterus and just worked its way out. This could be something that happened around the time of insertion, or may be related to the size, angle, or conditions like fibroids that can cause the uterus to have an irregular shape. For people who have an IUD expulsion, the chance of expelling a second IUD may be higher—in the 20% range (up to 30% in some studies).
If you want a second IUD after the first one came out, consider asking your health care provider about inserting the second IUD while using an ultrasound machine to make sure the IUD is inserted all the way to the top of the uterus where it belongs.
Want to learn more?
Does the non-hormonal/copper IUD (Paragard) cause copper toxicity?
IUDs are safe for most people with a uterus, and copper toxicity is super rare. That said, it can happen, especially in people with Wilson’s Disease, a rare genetic condition (about 1 in every 30,000 to 40,000 people have it) that affects your body’s ability to process copper. Given how low the daily dose of copper is from the non-hormonal IUD, it is extremely unlikely that someone who does not have Wilson’s Disease would experience copper toxicity.
Want to learn more?
What should I do before stopping my birth control?
If you’d like to stop your birth control and try to get pregnant, you can get pregnant pretty quickly after stopping most methods.
If you’re just not vibing with your choice of birth control, it might be time to switch things up! Before you do, ask yourself some questions to make sure you know what’s not working and what you might want in a new method. Thinking about why you want to switch methods and what your needs are going forward will help you figure out next steps that work for you.
If you’d like to stop your birth control and try to get pregnant, you can get pregnant pretty quickly after stopping most methods.

Heat up your weekends with our best sex tips and so much more.