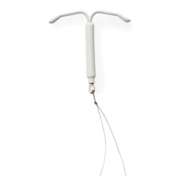
Those Mirena lawsuit ads: Fact and fiction
Because you deserve the full story about Mirena IUD risks and side effects.
The recent slew of Mirena IUD lawsuit ads are creepy. But are they true? We’re going to fearlessly wade into the scary things these ads claim, because we think the over 2 million U.S. women now using IUDs deserve the real info—without the hype.
What problems are being reported—and how common are they?
Some of the ads say 47,000 women have had problems with the Mirena. But where does that number come from? The Food and Drug Administration (FDA) scrutinizes drugs and devices for safety before they can be sold in the U.S., then continues collecting information about problems people have with drugs and devices after they’re on the market and being used more broadly.
Anyone can report problems to the FDA. Since Mirena came on the market in 2001, the FDA has received about 47,000 reports of problems with it. Many millions of women have used a Mirena over the 12 years it’s been on the market, so this number is actually a small fraction of the total—and it includes common complaints in addition to the rarer, scarier problems the lawsuit ads often focus on.
Here’s how the problems break down (and more about each below):
almost half (45%, or about 21,500 women) of the complaints are about IUD expulsion
pain during or after the IUD placement makes up 25% of the complaints (or 11,700 women)
complaints about more bleeding make up 21% (or 10,100 women)
complaints of less bleeding or no period account for 6% (or 2,800 women)
complaints of pregnancy with the IUD make up 5% (or 2,200 women)
perforation of the uterus accounts for 3% of the complaints (or 1,300 women)
Let’s look at the scientific evidence about how common each problem is and what it means if it happens to you.
Expulsion
It’s not surprising that almost half of the reported problems with Mirena were expulsion—it’s relatively common, occurring in up to 8% of women who get an IUD. Expulsion is a fancy way of saying that an IUD has been pushed out of its ideal location at the top of the uterus. The uterus is one big muscle, so this sometimes happens. In a complete expulsion, the IUD is pushed all the way out of the uterus into the vagina. In a partial expulsion (a.k.a. dislocation), an IUD is pushed only part way out and a woman may not know that her IUD isn’t where it should be.
If a woman doesn’t recognize a partially expelled IUD, it can mean the IUD isn’t working to prevent pregnancy. Signs of a partial expulsion include cramping, pain, and feeling the plastic of the IUD at the top of the strings. This is why doctors often advise checking on the IUD strings. If recognized quickly, a partial expulsion is not a big problem: the IUD needs to be removed, and a woman can decide if she wants to try another IUD or switch to a different method. After expelling one IUD, there may be a higher chance of expelling the next one.
The bottom line: Expulsion can be uncomfortable—and it’s definitely inconvenient—but it does not have lasting effects or cause infertility as some of the Mirena lawsuit ads imply.
Pain and bleeding
During insertion: IUD insertion pain is worse for some women than for others. (Even for women who experience a lot of pain during insertion, they often say it was worth the gain of hassle-free birth control.) After the IUD has been inserted, continuing pain may be a sign of a partial expulsion or another problem, so if the pain doesn’t go away within a few days of insertion, it’s definitely a good idea to check in with a health care provider.
During periods: In the long run, many women using a Mirena experience less period pain than they did before getting the IUD. About one-third of users have frequent or longer bleeding in the first three months, and about two-thirds have some spotting or bleeding between periods. After a year, about three-quarters of women have infrequent or no bleeding at all. On the other hand, some of the problems women report to the FDA are about lighter or nonexistent periods. Some Mirena users see this as a benefit, but if you’re not prepared for these possible changes, they can seem like a problem.
The bottom line: Only you know what’s normal for your body in terms of pain and periods. Learn as much as you can about how your pain and bleeding might be affected by any type of IUD before trying one. If after your IUD is inserted you have pain or bleeding beyond what you expected, talk to your health care provider.
Perforation and migration
For about 1 in 2,000 women, the IUD can get stuck in or puncture the uterus—also known as perforation. A U.S. woman aged 20-39 is more than 10 times more likely to have a stroke (12 in 2,000) than to experience perforation. Perforation only happens when the IUD is being put in. Highly skilled providers who have inserted many IUDs are less likely to have perforations. Women who are breastfeeding or have given birth within the last month are more likely to experience perforations because the muscle of the uterus is softer at those times.
What does it mean if there is a perforation? If it’s recognized immediately, the health care provider will stop the insertion. It takes about a week for the uterus to heal, and then a woman can have another IUD inserted if she wants. More than half of perforations may go unrecognized at the time of insertion. That may mean that a woman thought she had great birth control when she may not have. If undiagnosed for months, a perforation can make removing the IUD difficult, and can sometimes require surgery. Even in the worst-case scenario of an undiagnosed perforation that requires surgery, it shouldn’t have an impact on the woman’s future fertility.
Many of the lawsuit ads warn of IUDs migrating outside the uterus. Although it is extremely rare, there have been cases when an IUD has gotten past all of the thick layers of muscle of the uterus and entered the body cavity. How rare is this? So rare that even with tens of millions of women using IUDs worldwide, we can’t estimate how often it happens. We just know that there have been case reports in medical journals.
The bottom line: Perforation is rare and, if it’s recognized quickly, it’s not a major health event. Many providers will have you come back 4-6 weeks after an IUD placement to check on the strings and make sure everything is okay. If you’re worried, you can check your own strings. If you can’t find your strings, see your health care provider.
Pregnancy, now and later
Can you get pregnant with an IUD? Unfortunately, method failure is a risk with any and all contraceptives. So, yes—for a very small number of women, the IUD can fail and an accidental pregnancy can result. For the Mirena, this happens for about 2 in 1,000 women. That’s way less common than 90 pregnancies in 1,000 women using the pill—but it’s not zero.
What about getting pregnant after having an IUD? Studies have repeatedly shown that in the year after removing an IUD, over 80% of women who want to have a baby do get pregnant—exactly the same as for women who have never used an IUD. In other words, using an IUD now has no impact on future motherhood.
The bottom line: IUDs fail way less than other kinds of birth control, and they don’t affect your ability to get pregnant in the future.
Serious problems with IUDs are rare—but we understand that’s small comfort if you or someone you care about experiences them. Each person has to weigh the risks and benefits when making any decision, including about birth control, and we hope that this and our other information about IUDs helps create a more complete picture than the lawsuit ads alone.
How do you feel about this article?

Heat up your weekends with our best sex tips and so much more.