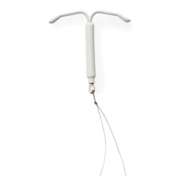
No pain, no gain: The IUD insertion process
Unlike me, you should take some advance measures to prepare yourself for the process.

By Lena Chen. A version of this article was originally published on November 11, 2009, on SexReally.com.
I wish I could say that getting the IUD was easy once I made my decision that the love affair with the pill was over. In reality, it took me three visits before I finally baby-proofed my uterus. First my doctor wanted me to get a pap smear and STI test. An abnormal pap result delayed my efforts further. After a lab test determined that some cervical lesions were low-grade and no cause for alarm, I finally found myself face-to-face with a foot-long box containing my IUD. Thankfully, the size was misleading.
The Mirena IUD is actually less than 1.5 inches long. Still, that little device was responsible for the most painful experience of my life and I say this as someone who’s gotten five piercings and a tattoo. Forgoing anesthesia and prescription painkillers, I whimpered with my boyfriend by my side as the doctor fit the IUD into place. I felt intense cramps (similar to contractions, I imagine) the second it entered my body. Utterly shaken by the invasion of this foreign object, my legs trembled and my teeth chattered uncontrollably. I gripped my boyfriend’s hand and whispered, “Remind me to get a C-section if I ever decide to have kids.”
That’s probably as close an approximation of childbirth as I’ve ever experienced, but I don’t have any complaints about the IUD now that the initial ordeal is over. Despite a crampy first week and spotting (which can last for several weeks), I’ve been pretty pleased with the IUD, which has rendered the pesky birth control pill unnecessary. Total cost for five years of a worry-free womb? $0. My insurance policy covers the device and the insertion procedure entirely. Compare that to $480 for five years of my generic pill.*
Unlike me, you should take some advance measures to prepare yourself for the insertion. One of my friends, who got the IUD a month after she gave birth to her first child, claimed that it even hurt more than labor. Conversely, I heard from many other women that insertion was no more uncomfortable than a pap smear. In my opinion, better safe than sorry either way. Unless you’re certain you can withstand a lot of pain, going the all-natural route might lead to a rude cervical awakening.
Here are a few things that may help you avoid my experience:
Say yes to drugs. I’m so wary of over-the-counter medication abuse that I don’t even take ibuprofen for headaches, but in the days following my IUD, painkillers were the only effective weapon against severe cramping that would have otherwise left me incapacitated. After your appointment, keep Midol handy, or any painkillers that target lower abdominal pain and menstrual symptoms. You can also try taking painkillers before your insertion appointment.
Welcome Aunt Flo. Schedule your appointment to coincide with your menstrual cycle since your cervix will already be slightly dilated then. Don’t worry about what your gynecologist will think about the mess. They’re used to it and many will probably recommend waiting until your period anyway.
Rough sex is out of the question. (At least for the first week.) Your cervix won’t appreciate head-on collisions for a while. Though I only needed a couple weeks to recover, one of my friends said penetrative intercourse was uncomfortable for the first month. If you can’t wait, either try to take it easy or be prepared to feel crampy in the afterglow.
Heat up. Self-heating stick-on pads (the kind you can get at drugstores for sports injuries or menstrual pain) may help alleviate discomfort throughout the day. At home, a hot water bottle or an electric blanket will also do the trick.
There are other birth control methods that don’t require an uncomfortable insertion process, but for many women the IUD causes relatively few side effects and works really well for years. Hormonal IUDs, which release progesterone, are relatively low-hormone compared to other forms of hormonal contraception. If you think you can brave the gynecologist’s table, look into the IUD. It’s affordable, widely available, and foolproof.
*Editor’s note: This article was written before the Affordable Care Act made it a requirement for insurance companies to cover all FDA-approved birth control methods without out-of-pocket costs. Today, both the IUD and generic pills would be covered. Sometimes change is good!
—
Lena Chen is a blogger, writer and speaker on sex, gender and feminism. Her writing has been featured in The New York Times and Newsweek.
How do you feel about this article?

Heat up your weekends with our best sex tips and so much more.